|
Vitamin C was discovered in 1912, isolated in 1928, and in 1933, was the first vitamin to be chemically produced. It is on the WHO's list of essential medicines, the safest and most effective medicines needed in a health system. Foods containing Vitamin C include Citrus fruits, Kiwi, Guava, Broccoli, Brussels sprouts, bell peppers and Strawberries. Vitamin C is available as an inexpensive generic and over-the-counter medication.
Benefits of Vitamin C: IMMUNE BOOSTER Vitamin C claims to improve your immunity, it can help in fighting infections like colds and the flu. POTENT ANTIOXIDANT DRUG Vitamin C protects your cells from reactive oxygen species (ROS) and decreases oxidative damage that leads to photoageing and disease. COLLAGEN SYNTHESIS Vitamin C is essential for collagen biosynthesis. Influences both the quality and quantity of collagen produced. Collagen makes your skin more youthful and firm. GLOWING AND HEALTHY SKIN Reduces signs of ageing like wrinkles, discolouration and sagging skin. Topical Vitamin C decreases melanin formation its used as depigmentation agent and it also gives good glow to your skin. HEALTHY HEART Lowers “bad” cholesterol (LDL cholesterol levels). Daily supplement can protect you from fatal heart conditions. PREVENTS ANEMIA Anemia is a condition in which there is deceased red blood cells in the blood stream, most common is iron deficiency anemia. Vitamin C improves iron absorption almost 70 percent. If you are anemic make sure you take vitamin C. EASES GOUT OUT May prevent gout and gout flare ups by breaking down the build-ups of uric acid. PROTECTS AND SUPPORTS MEMORY Scientists believe oxidative damage is one of the factor that leads to memory loss disorders. Vitamin C may help to reduce age related cognitive diseases and could even improve memory and cognitive function in those with dementia. WOUND HEALING Vitamin C has good anti-inflammatory activity; it may help in wound healing making it a popular ingredient in natural cleansing solutions. Vitamin C is also used in skin condition such as acne and rosacea for its anti-inflammatory properties. HEALTH AND FAMILY WELFARE DEPARTMENT recommends Vitamin C, Zinc and herbal powder (Nilavembu and Kabasura Kudineer) supplementation as an important measure to improve your immunity against COVID infection (especially for the front-line staff and others in COVID-19 duty).
0 Comments
Inspite of avoiding pollution and makeup why is our skin breaking out?
The culprit "CORONA" has brought stress in our lives, due to which our body releases cortisol which is a steroid hormone. When your cortisol level goes up, it prompts your skin to produce excess sebum. This is when the oil clogs the pores and causes inflammation that leads to acne (pimple) formation. Tips to prevent lockdown acne breakout:
DO THE FIVE to HELP STOP CORONAVIRUS
What is eczema or dermatitis? The term “eczema” and “dermatitis” is used interchangeably, it refers to inflammation of the skin. Eczema is one of the most common causes of dry, sensitive skin. This is an itchy and inflamed rash that the affected person scratches persistently. Atopic Eczema: It is the most common type of eczema. There are many other type of eczema as well. Almost everyone who has eczema experience similar symptoms. The following are some of the other types of eczema. Contact Dermatitis: There are two main types of Contact dermatitis – allergic and irritant type. Allergic contact dermatitis is caused by a specific hypersensitivity to a material such as rubber, fragrance, cement, parthenium (plant), nickel, glue, etc. Irritant contact dermatitis is caused by exposure to irritating substances such as soap, detergent, bleach, insect secretion, etc. Avoidance of the allergen or irritant is the first step required in the treatment. Seborrhoeic dermatitis: This is the most commonly seen in babies and young adults. It is seen on oily areas of body like the scalp, face, upper chest, and back. It appears as yellow scaly rash on the affected areas, on scalp it appears as dandruff. Discoid Eczema: It presents with coin shaped, itchy and scaly patches which tends to ooze. Asteototic eczema: It appears in the form of extreme dryness of the skin. The rash looks like “cracked titles on the floor”, especially seen over the forearm and legs of elderly individuals. Stasis eczema: It is commonly seen in elderly and people with varicose veins on the legs. The pooling of blood in the leg veins due to gravity leads to formation of this type of eczema. How do I care for the skin?
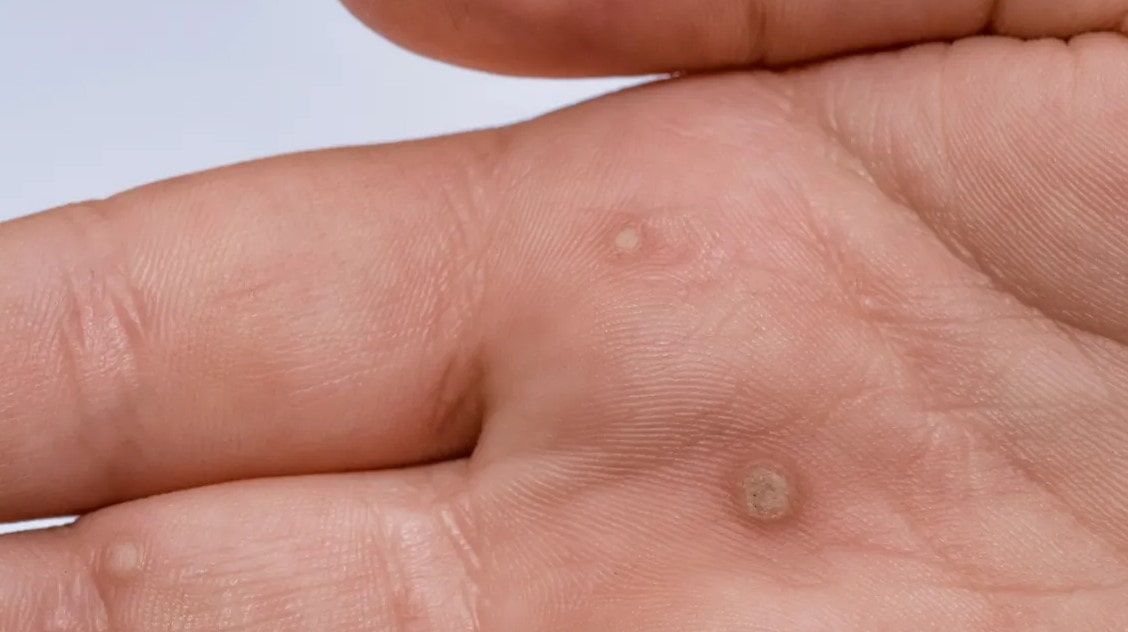
What causes Warts?
Warts are skin growth caused by a virus. Warts are common and can be a nuisance. They can grow on any part of the body like face, neck, on the fingers, along the forearm or on the pressure areas like palms or the sole. How do they look? Warts have a rough surface on which tiny dots may be seen. They may appear as projecting growth on face and neck. On the sole they grow inward, pressure of standing and walking may cause pain. Are warts contagious? Yes, warts are contagious and may spread from one part of the body to another or to other people. What is the perfect solution for Warts? There is no perfect treatment for warts. Treatment consists of destroying the outer layer of skin where the wart grows on. This can be done by electrosurgery, laser, cryotherapy or with topical chemical solutions. The treatment depends on the location and size of the warts and clinical judgement of the dermatologist. No matter what treatment is used, warts occasionally fail to disappear. There is no need to worry if a wart recurs; just consult your dermatologist for further therapy. Dark circles/ periorbital melanosis is a common condition and an ill defined entity. It appears as brownish-black pigmentation around the eyelids. It not only gives a tired look to the patient but also gives a negative impact on their quality of life.
The causes of dark circles includes:
Wide range of topical creams and serums, chemical peeling, LASER treatment, fillers, PRP, are available as treatment options depending on the cause of the dark circles. Additionally your dermatologist may suggest sun protection and lifestyle modifications such as adequate sleep, hydration, and diet to achieve an optimal result. What causes psoriasis?
The exact cause of psoriasis is unknown. However, it is understood that the immune system, environmental factors and family history can play critical roles in its development. The immune system is somehow triggered, which causes a series of events such as inflammation, acceleration of skin cell growth, etc. It is important to understand that psoriasis is not contagious. A person cannot “catch” it by touching the affected individual. How widespread is psoriasis? Psoriasis is a common inflammatory condition that affects about 2% of the world population. Prevalence in India varies between 0.8% to 2.8%. How is psoriasis diagnosed? The diagnosis of psoriasis is usually made by a dermatologist examining the affected skin for typical signs of the disease and obtaining an appropriate patient history. In some cases, to aid in the diagnosis, your dermatologist may obtain a small sample of skin and examine it under a microscope. What triggers psoriasis to flare? Certain things may cause exacerbation of pre-existing psoriasis or may trigger psoriasis. Among these are stress, skin injuries, throat infections, and reactions to certain medications. Weather can also worsen psoriasis, especially in cold and dry climates. Is psoriasis curable? At present, there is no known cure for psoriasis. However, there are certain medications which can control and help to treat psoriasis. It is important for patients to speak with their dermatologists about appropriate treatment(s) that may effectively manage their psoriasis. Treatment may include medications applied to the skin, phototherapy, medications taken orally or given by injection. Vitiligo is the most common depigmenting disorder having a major impact on the quality of life of patients. There are no other textural changes besides loss of color. Studies have shown that there is link between diet, nutrition level and vitiligo.
What to avoid?
What can be beneficial?
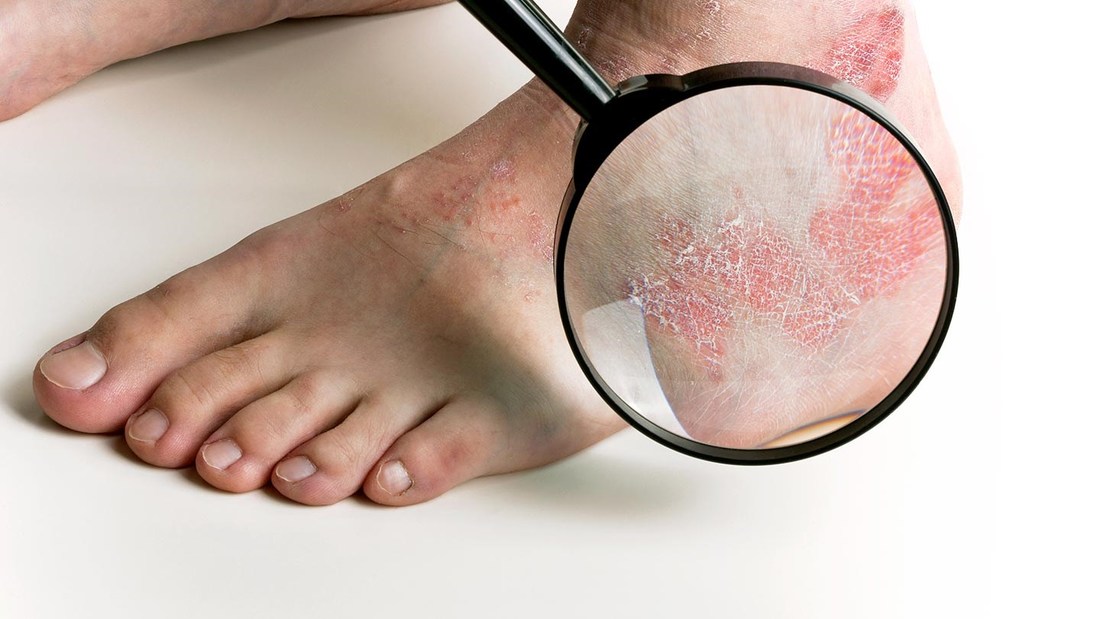
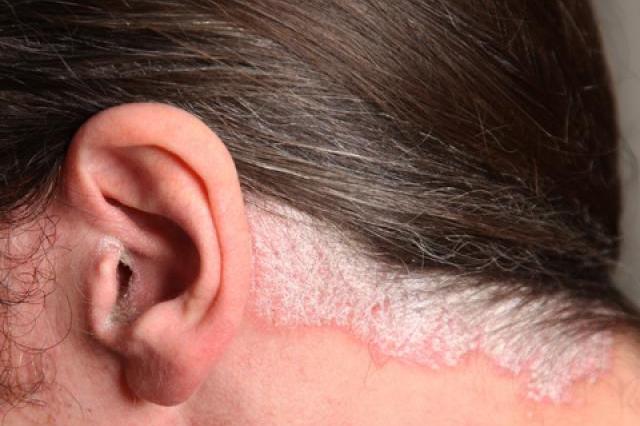
Psoriasis is a common, chronic, inflammatory, multisystem disease of the skin and joints. Scalp is the first site of involvement in up to 25% of the patients of psoriasis. Up to 79% of patients of chronic plaque psoriasis may have scalp involvement. It can be mild to severe, and often itchy, cosmetically embarrassing and affects the quality of life adversely.
Scalp psoriasis can be very mild, with slight scaling. It can also be very severe with thick, crusted lesions covering the entire scalp. Psoriasis can extend beyond the hairline onto the forehead or the back of the neck. Other skin disorders, such as seborrheic dermatitis, may look similar to psoriasis. How to differentiate between scalp psoriasis and seborrheic dermatitis of the scalp?
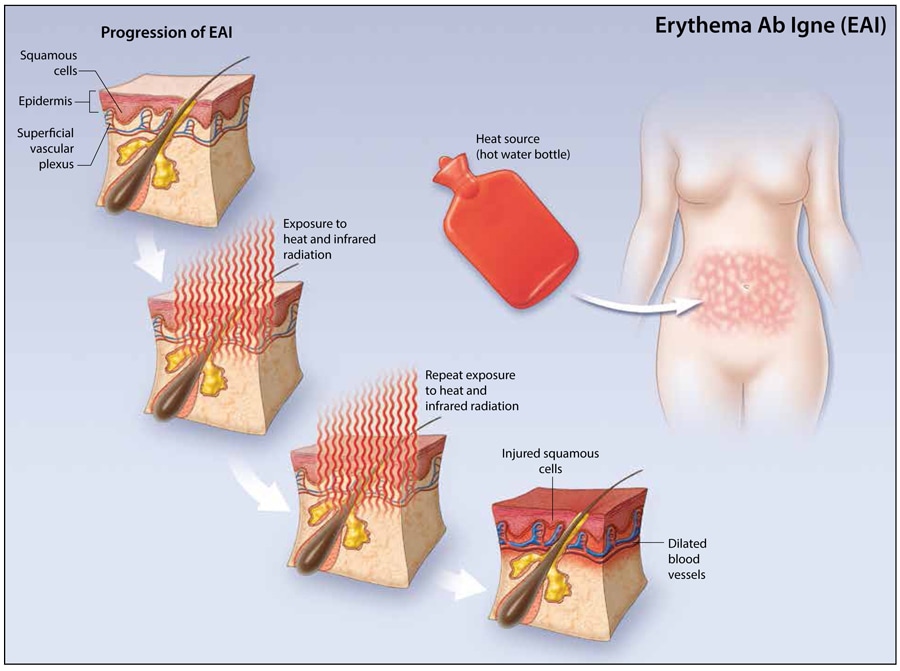
A combination of treatment (shampoo, lotion, UV light) will be advised to a person with scalp psoriasis, sometimes the treatment will be rotated since it becomes less responsive to medications after repeated use. Systemic medication may be used if psoriasis is present elsewhere on the body and/or the scalp psoriasis is moderate to severe. Toasted skin syndrome is characterized as localized areas of reticulated (net-like) reddness and dark pigmentation due to chronic and repeated exposure to infrared radiation. Main cause is repeated exposures to heat at a lower level than that which causes a thermal burn. Other terms used to describe toasted skin syndrome include erythema ab igne, ephelis ignealis, erythema ab calore and fire stains.
Who can develop this syndrome?
Can it be treated?
Nail cuticle is a thin layer of dead tissue riding on the nail plate and forms a seal. It prevents entry of pathogens from infecting the nail matrix.
What happens if your nail cuticle is damaged by external irritants or removed?
How you can protect your nail cuticle?
|
AuthorDr.S.Nagakeerthana is a consultant dermatologist and dermatosurgeon. Archives
April 2020
Categories
All
|
- Home
- About
- Services
- Gallery
-
Common Conditions
- Acne
- Alopecia areata
- Atopic Dermatitis / Eczema
- Calluses and Corns
- Cellulitis
- Cysts
- Dandruff
- Dry Skin
- Fungal Infections
- Premature Hair Graying
- Hair Loss
- Hives (urticaria)
- Impetigo
- Keloid
- Lichen Planus
- Psoriasis
- Pityriasis Rosea
- Rosacea
- Scabies
- Seborrheic Keratosis
- Shingles (Herpes Zoster)
- Skin Cancer
- Skin Tags
- Vitiligo
- Warts
- Yeast Infection
- Blog
- Contact
|
|
Dr. S. Nagakeerthana M.D. DVL NK Skin Hair & Laser Centre No: 9, Kasiviswanathar north st, Kumbakonam, Tamil Nadu 612001.
|
Speciality Skin Care Treatments
|







 RSS Feed
RSS Feed