|
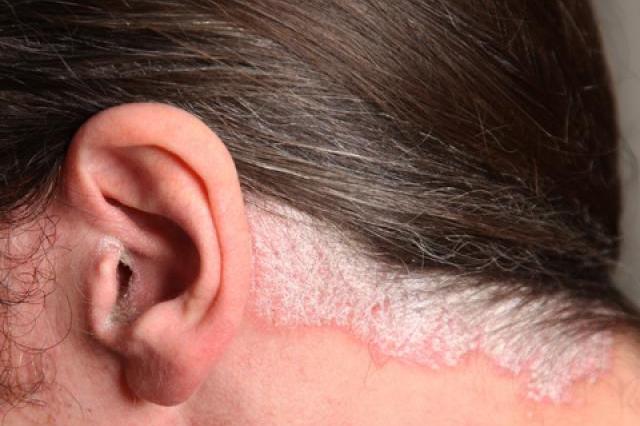
Psoriasis is a common, chronic, inflammatory, multisystem disease of the skin and joints. Scalp is the first site of involvement in up to 25% of the patients of psoriasis. Up to 79% of patients of chronic plaque psoriasis may have scalp involvement. It can be mild to severe, and often itchy, cosmetically embarrassing and affects the quality of life adversely.
Scalp psoriasis can be very mild, with slight scaling. It can also be very severe with thick, crusted lesions covering the entire scalp. Psoriasis can extend beyond the hairline onto the forehead or the back of the neck. Other skin disorders, such as seborrheic dermatitis, may look similar to psoriasis. How to differentiate between scalp psoriasis and seborrheic dermatitis of the scalp?
A combination of treatment (shampoo, lotion, UV light) will be advised to a person with scalp psoriasis, sometimes the treatment will be rotated since it becomes less responsive to medications after repeated use. Systemic medication may be used if psoriasis is present elsewhere on the body and/or the scalp psoriasis is moderate to severe.
0 Comments
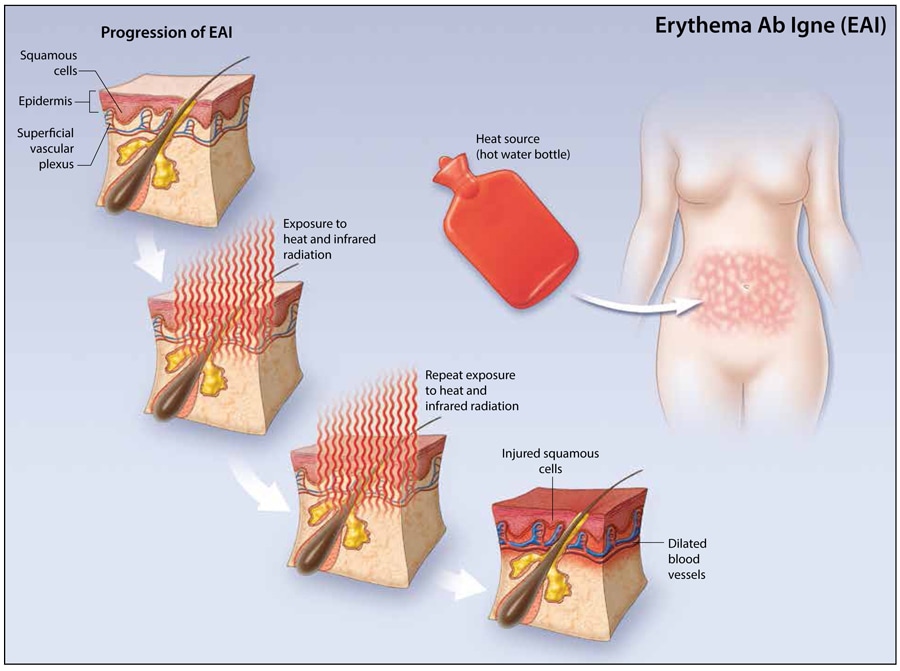
Toasted skin syndrome is characterized as localized areas of reticulated (net-like) reddness and dark pigmentation due to chronic and repeated exposure to infrared radiation. Main cause is repeated exposures to heat at a lower level than that which causes a thermal burn. Other terms used to describe toasted skin syndrome include erythema ab igne, ephelis ignealis, erythema ab calore and fire stains.
Who can develop this syndrome?
Can it be treated?
Nail cuticle is a thin layer of dead tissue riding on the nail plate and forms a seal. It prevents entry of pathogens from infecting the nail matrix.
What happens if your nail cuticle is damaged by external irritants or removed?
How you can protect your nail cuticle?
Avoid removing the mole if it is given as an identification mark for government documents such as passport, ration card, etc.
If you have tendency to develop keloids or hypertrophic scars then invasive procedures must be avoided. Mole with irregular margin and colour should be further analysed to rule out melanoma. Mole removal can leave behind a scar or pigmentation especially when it is big or deep. You must follow up after suture removal, your dermatologist may suggest you topical medication to make your scar less prominent. Remember, your mole can regrow from the little remnants which may have been left behind. Deeper moles have high chance of regrowth, in such cases multiple sittings may be required for complete removal. |
AuthorDr.S.Nagakeerthana is a consultant dermatologist and dermatosurgeon. Archives
April 2020
Categories
All
|
- Home
- About
- Services
- Gallery
-
Common Conditions
- Acne
- Alopecia areata
- Atopic Dermatitis / Eczema
- Calluses and Corns
- Cellulitis
- Cysts
- Dandruff
- Dry Skin
- Fungal Infections
- Premature Hair Graying
- Hair Loss
- Hives (urticaria)
- Impetigo
- Keloid
- Lichen Planus
- Psoriasis
- Pityriasis Rosea
- Rosacea
- Scabies
- Seborrheic Keratosis
- Shingles (Herpes Zoster)
- Skin Cancer
- Skin Tags
- Vitiligo
- Warts
- Yeast Infection
- Blog
- Contact
|
|
Dr. S. Nagakeerthana M.D. DVL NK Skin Hair & Laser Centre No: 9, Kasiviswanathar north st, Kumbakonam, Tamil Nadu 612001.
|
Speciality Skin Care Treatments
|


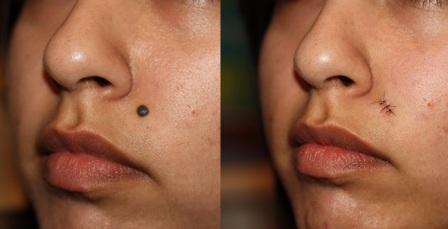
 RSS Feed
RSS Feed